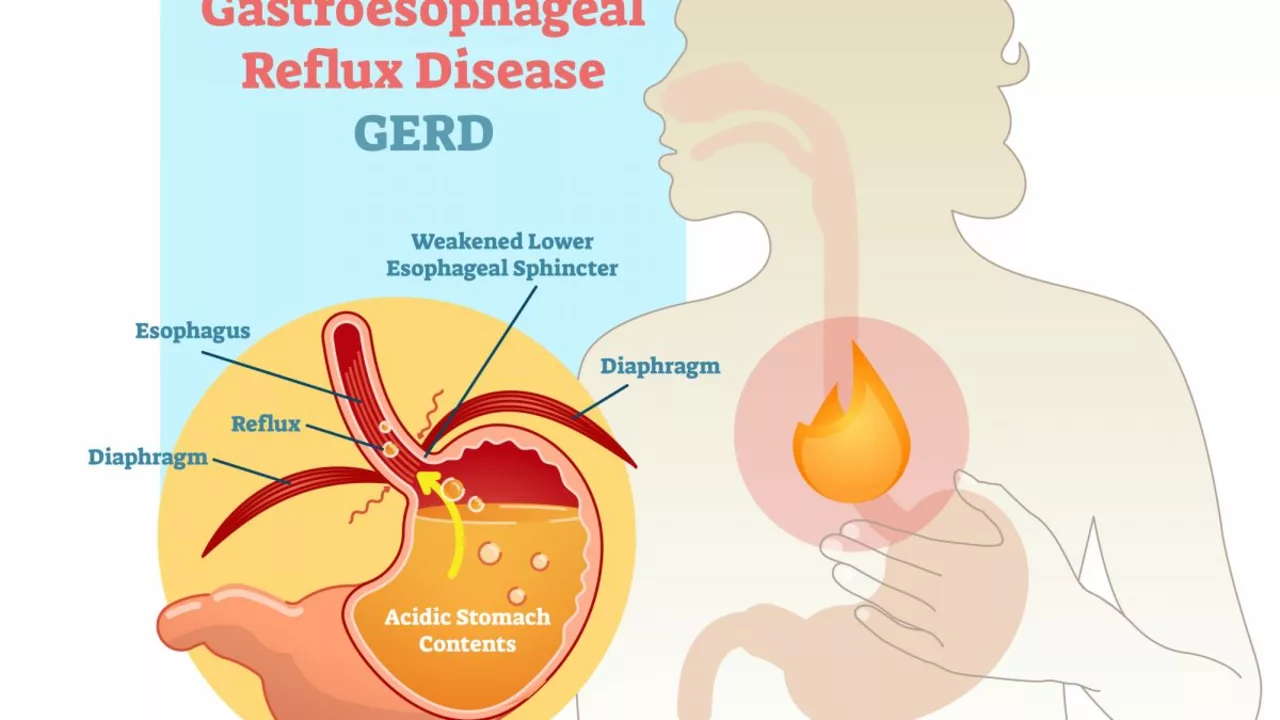
GERD: Practical Steps to Ease Acid Reflux Today
Heartburn waking you at night or after meals? GERD (gastroesophageal reflux disease) is common, but some simple changes usually help. This page gives clear, practical tips—what to try at home, how medicines work, and when you should see a doctor.
First, know your triggers. Fatty foods, coffee, chocolate, peppermint, spicy meals and alcohol often make reflux worse. Keep a short food diary for two weeks: note what you eat and when symptoms start. Also watch timing—lying down within two hours after a meal is a huge risk. Try finishing dinner earlier and avoid late-night snacking.
Quick at-home fixes
Raise the head of your bed 6–8 inches or use a wedge pillow so gravity keeps acid down while you sleep. Lose even a little weight if you’re overweight; a 5–10% drop often cuts symptoms. Stop smoking and limit alcohol—both relax the lower esophageal sphincter. Eat smaller, more frequent meals and chew slowly. Over-the-counter antacids can give fast relief for occasional heartburn. H2 blockers (like famotidine) reduce acid for several hours and are useful for mild cases.
When meds or a doctor are needed
If symptoms happen more than twice a week or interfere with sleep, proton pump inhibitors (PPIs) such as omeprazole or pantoprazole often work better. The 2025 GERD guidelines recommend starting with the lowest effective PPI dose for 4–8 weeks, then reassess. Long-term PPI use can be safe but discuss risks and benefits with your doctor—do not stop suddenly without medical advice. If medicines don’t help, or you have trouble swallowing, unintentional weight loss, persistent vomiting, or black stools, get evaluated urgently—these are red flags.
Think about medications you take. NSAIDs, certain blood pressure drugs, and some asthma medicines can worsen reflux. Tell your clinician about all prescriptions and supplements so they can adjust therapies if needed.
For chronic GERD, lifestyle changes plus targeted meds work for most people. Some need endoscopic procedures or surgery when medical therapy fails. Ask for a referral to a gastroenterologist if two courses of PPI therapy don’t control symptoms or if testing like endoscopy or pH monitoring is suggested.
Useful note: if you’re comparing PPIs, omeprazole and pantoprazole are similar in strength but differ in drug interactions and cost. Generic versions make treatment affordable. Our site has articles comparing online pharmacies, costs, and safe ways to buy meds—check our omeprazole and 2025 guideline posts for details.
Practical meal ideas: opt for grilled chicken, steamed vegetables, oatmeal, bananas, and non-citrus fruits. Avoid tomato sauce, citrus juices, fried foods, and large portions. If you use a PPI, take it 30–60 minutes before your main meal for best effect. Try switching to low-acid coffee or decaf and go for herbal teas like ginger or chamomile. Keep water handy but sip — big gulps can worsen reflux. Small consistent changes beat dramatic diets. Ask questions, stay curious.
Take action: track triggers, adjust meals and sleep position, try OTC options for mild reflux, and see a clinician when symptoms are frequent or severe. Small, consistent steps often bring big relief.
The Impact of GERD on Quality of Life: How Gastroesophageal Reflux Disease Affects Daily Living
As someone who suffers from GERD, I can attest to the impact this condition has on daily life. The constant heartburn, regurgitation, and chest pain make even simple tasks challenging. Due to disrupted sleep patterns, many of us also experience fatigue, which affects our productivity and mood. Additionally, GERD sufferers often have to make significant dietary adjustments to manage symptoms, which can be frustrating and isolating. In summary, GERD significantly impacts our quality of life, making everyday activities more difficult and limiting our food choices.