Allergies: Simple Ways to Spot Them and Feel Better Fast
Sneezing, itchy eyes, a rash, or sudden swelling—those can be signs of an allergy. Allergies happen when your immune system overreacts to otherwise harmless things: pollen, dust mites, pet dander, certain foods, insect venom, or medicines. Symptoms range from mild irritation to life-threatening reactions, so knowing what to do matters.
Common symptoms and when to act
Runny nose, sneezing and itchy eyes usually point to seasonal or indoor allergies. Hives, stomach upset, or swelling after eating suggest a food allergy. Trouble breathing, tight throat, fainting, or rapid pulse could mean anaphylaxis—a medical emergency. If you or someone near you shows those severe signs, use an epinephrine auto‑injector if available and call emergency services immediately.
Quick relief options
For everyday symptoms, start with simple steps: antihistamine pills like cetirizine, loratadine or fexofenadine relieve sneezing, itching and hives without heavy sedation. Nasal steroid sprays (fluticasone, budesonide) cut nasal congestion and inflammation but take a few days to reach full effect. For itchy, red eyes try an antihistamine eye drop. Use oral decongestants only short-term and avoid them if you have high blood pressure unless your doctor says it’s OK.
If food or drug allergies are suspected, stop the trigger and see your doctor before retrying anything. For repeated or unclear symptoms, an allergist can run skin prick tests or blood tests to confirm the cause and suggest treatment plans.
Allergy shots or sublingual tablets (immunotherapy) are real options if medication and avoidance don’t work. They reduce sensitivity over months to years and can offer lasting benefit for pollen, dust mites, and some pet allergies.
For kids, dosing and choices differ. Don’t give over‑the‑counter meds to an infant without a pediatrician’s advice. Keep active prescriptions, like epinephrine, current and teach caregivers how to use them.
Prevention is often the fastest path to relief. Check pollen counts on high‑allergy days and stay indoors during peak times. Use HEPA filters, wash bedding weekly in hot water, keep pets out of bedrooms, and shower after being outside to wash off pollen. Read food labels carefully and ask about ingredients when eating out.
Traveling? Pack extra medication, a copy of your allergy action plan, and any emergency meds. If you have a known severe allergy, wear medical ID and make sure travel companions know how to help.
If symptoms don’t improve with OTC meds, get worse, or affect sleep and daily life, see a doctor. A clear diagnosis gets you the right treatment—fewer flare‑ups and better control. Small steps—smart meds, avoidance and an action plan—make allergies much easier to live with.
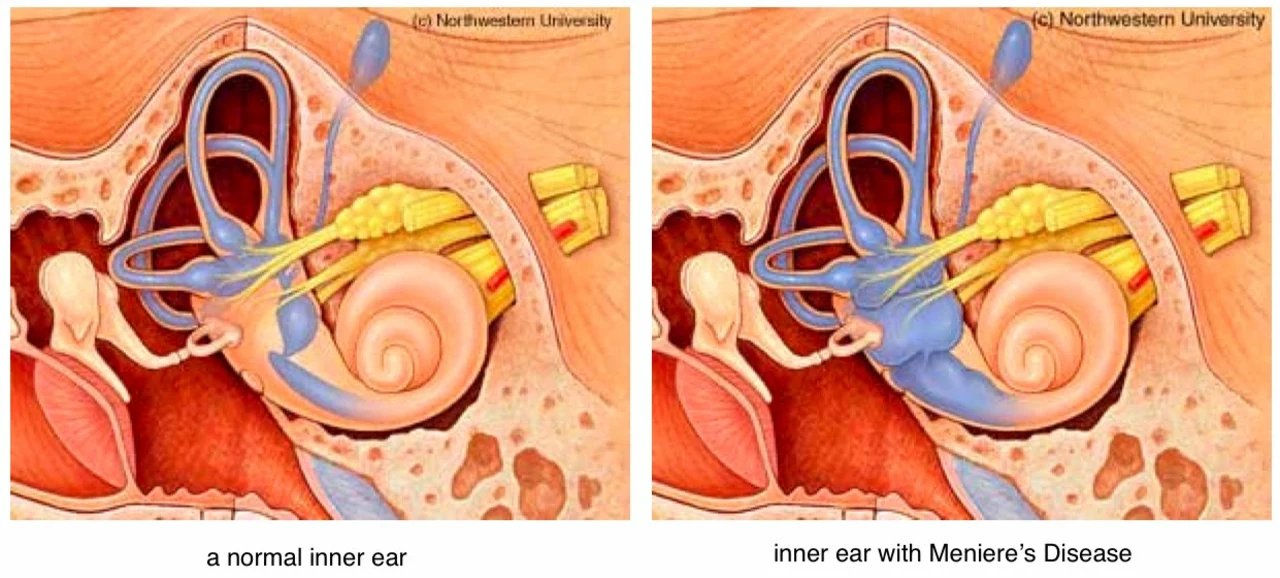
Meniere's Disease and Allergies: Is There a Link?
As someone who suffers from allergies, I've often wondered if there's a connection between them and Meniere's Disease. Recently, I've come across some information that points towards a possible link. It seems that both conditions involve the immune system and inflammation, which could be the common ground between them. Some studies even suggest that managing allergies might help alleviate symptoms of Meniere's Disease. I'm definitely interested in learning more about this connection and how it might impact my own health.