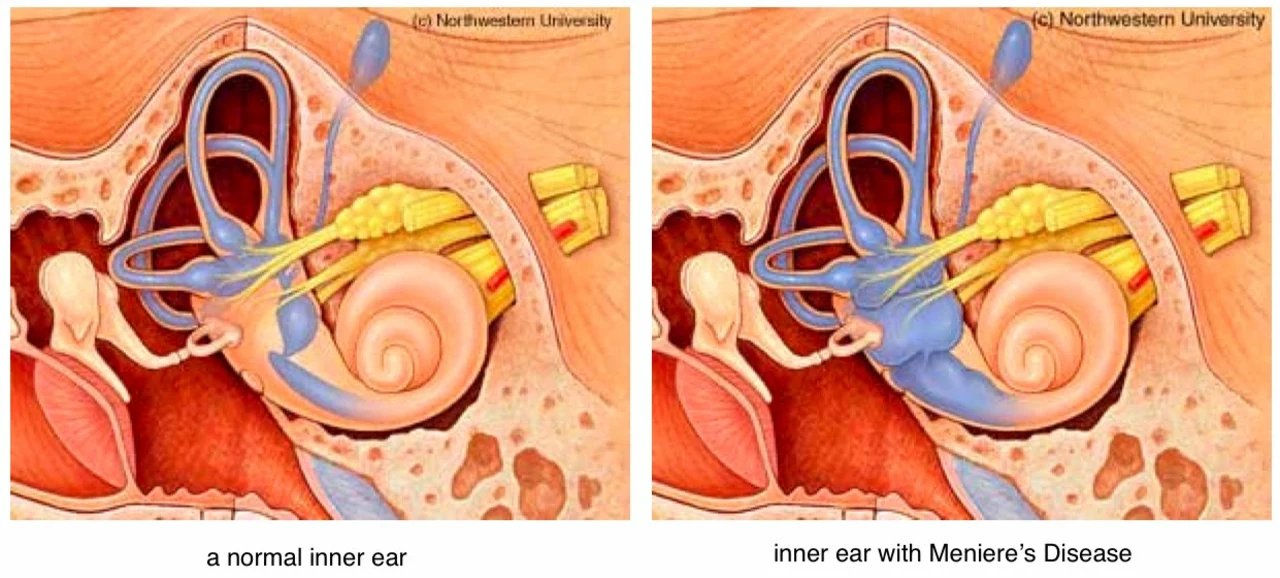
Meniere's disease: what to watch for and how to cope
Meniere's disease is an inner ear condition that causes sudden vertigo, hearing loss, and ringing in the ear. Attacks can be scary and unpredictable, but knowing the signs and simple strategies can help you stay in control. This page gives clear, practical steps for spotting symptoms, getting a diagnosis, and managing daily life.
Common symptoms and what they feel like
Vertigo is the hallmark symptom. It feels like the room is spinning and can last from minutes to hours. Nausea and balance problems often come with it. Hearing may shift during or after attacks, usually affecting one ear. Tinnitus — a constant or pulsing ringing — is common. Some people also report a feeling of fullness or pressure in the affected ear. Symptoms may come in clusters over weeks or months, then settle for a while.
Not every dizzy spell is Meniere's. If you have sudden, intense spinning plus hearing changes on one side, mention both to your doctor. Keeping a short attack log (time, length, triggers, symptoms) helps with diagnosis.
Causes, diagnosis, and treatments that actually help
Doctors think Meniere's comes from excess fluid in the inner ear. Triggers vary: salt intake, stress, caffeine, alcohol, and some medications can make attacks worse. Tests usually include a hearing test (audiogram), balance assessments, and sometimes MRI to rule out other problems. There's no single lab test that proves Meniere's, so your doctor will piece the story together from symptoms and tests.
Treatment focuses on reducing attack frequency and easing symptoms. During an attack, doctors can prescribe anti-nausea drugs and vestibular suppressants to help with spinning. For long-term control, many start with diet and lifestyle changes: cut salt, limit caffeine and alcohol, manage stress, and keep a sleep routine. Diuretics are commonly tried to reduce inner ear fluid. Injections of steroids or gentamicin into the ear are options if attacks remain frequent. Surgery is rarely needed but can be considered for severe, unresponsive cases.
Hearing loss may be gradual. Hearing aids can help and often improve quality of life. Vestibular rehabilitation (physical therapy for balance) teaches exercises that reduce dizziness between attacks. Cognitive strategies and therapy can also help when anxiety or fear of attacks becomes a problem.
Everyday tips: carry motion-sickness meds if you’ve had attacks, avoid driving during recovery, keep hydrated, and use a low-salt meal plan. Share your condition with close contacts so they know how to help during an attack. If you notice worsening hearing, frequent attacks, or new neurological signs like weakness or double vision, see a doctor right away.
Meniere's is unpredictable, but many people learn to manage it and keep a good life. Simple changes, the right medical steps, and practical planning make most days manageable.
Meniere's Disease and Allergies: Is There a Link?
As someone who suffers from allergies, I've often wondered if there's a connection between them and Meniere's Disease. Recently, I've come across some information that points towards a possible link. It seems that both conditions involve the immune system and inflammation, which could be the common ground between them. Some studies even suggest that managing allergies might help alleviate symptoms of Meniere's Disease. I'm definitely interested in learning more about this connection and how it might impact my own health.