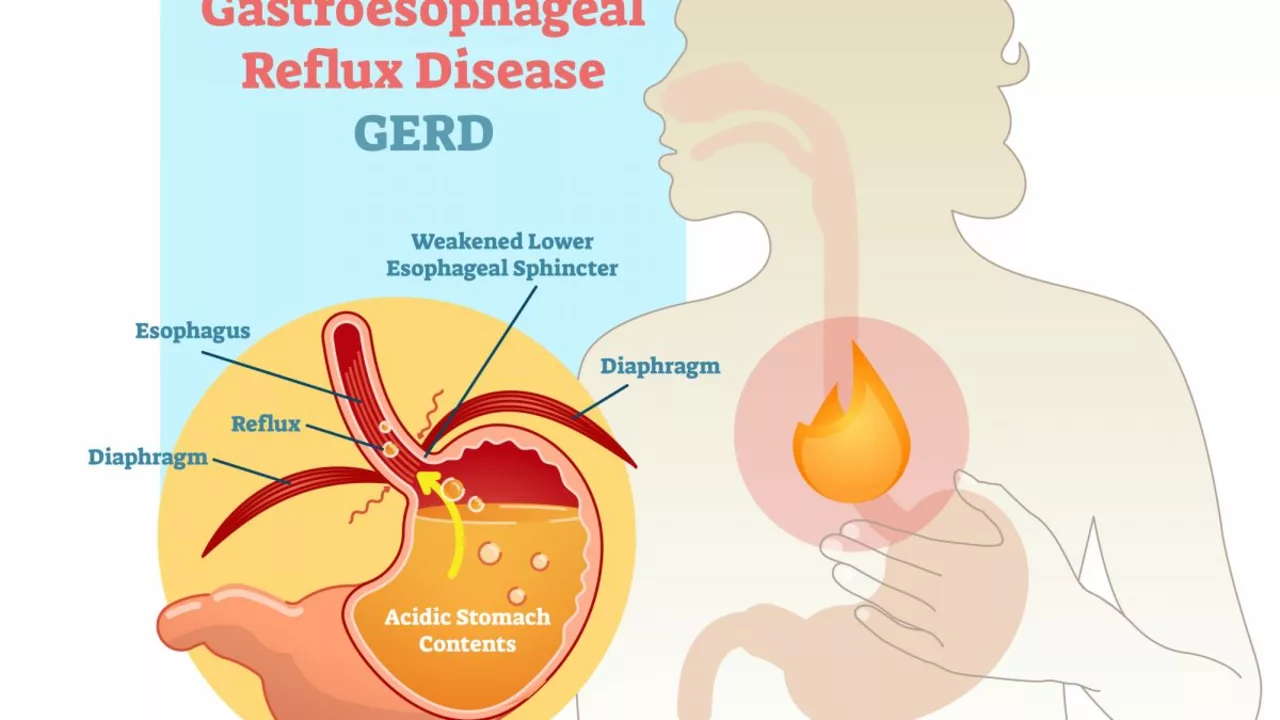
Gastroesophageal Reflux Disease (GERD): What to Watch For and What to Do
Heartburn once in a while is normal. Heartburn several times a week? That’s likely gastroesophageal reflux disease (GERD). GERD happens when stomach acid keeps moving up into the esophagus, causing burning, regurgitation, and sometimes cough or hoarseness. Symptoms can be mild or seriously annoying—either way, you don’t have to just live with it.
Spot the symptoms fast
Common signs include a burning feeling behind the breastbone, sour taste in the mouth, burping, and chest discomfort after meals. Less obvious signs are a chronic cough, hoarse voice, or trouble swallowing. If you notice weight loss, vomiting blood, or black stools, get medical help right away—those are alarm signals.
Causes vary. The lower esophageal sphincter (LES) normally keeps acid down; when it relaxes at the wrong times, reflux starts. Being overweight, smoking, pregnancy, and certain foods or medicines can weaken LES function. A hiatal hernia also makes reflux more likely.
Simple fixes you can try today
Start with lifestyle changes that actually work: lose a little weight if you’re overweight, don’t lie down within two to three hours after eating, and raise the head of your bed 6–8 inches. Eat smaller meals, avoid trigger foods like fried dishes, chocolate, peppermint, citrus, tomatoes, and heavy alcohol use. Chewing sugar-free gum after meals can help clear acid by stimulating saliva.
Over-the-counter options give quick relief. Antacids neutralize acid fast but don’t heal inflammation. H2 blockers (like famotidine) reduce acid for several hours. Proton pump inhibitors (PPIs) such as omeprazole and pantoprazole are more powerful; they’re best when symptoms are frequent or when healing of the esophagus is needed. Newer guidelines advise using the lowest effective dose and checking with your doctor about long-term need.
Tests make sense when symptoms don’t improve or when doctors worry about complications. An upper endoscopy looks for damage. Ambulatory pH testing measures acid exposure. Manometry checks swallowing and LES function. These tests guide treatments like surgery or device options (for people who don’t want lifelong meds).
Long-term PPI use can be fine for many people, but it’s worth discussing risks and benefits with your clinician. Some patients step down to H2 blockers or take PPIs only when needed. If lifestyle changes and meds don’t control symptoms, anti-reflux surgery or newer devices can be options to reduce reflux without daily pills.
If daily heartburn affects your sleep, work, or mood, start a conversation with your healthcare provider. Try the lifestyle tweaks for a few weeks, use OTC meds for symptom control, and see your doctor if things don’t improve or if alarm signs appear. Simple steps often make a big difference—and there are reliable treatment options if you need them.
The Impact of GERD on Quality of Life: How Gastroesophageal Reflux Disease Affects Daily Living
As someone who suffers from GERD, I can attest to the impact this condition has on daily life. The constant heartburn, regurgitation, and chest pain make even simple tasks challenging. Due to disrupted sleep patterns, many of us also experience fatigue, which affects our productivity and mood. Additionally, GERD sufferers often have to make significant dietary adjustments to manage symptoms, which can be frustrating and isolating. In summary, GERD significantly impacts our quality of life, making everyday activities more difficult and limiting our food choices.